Blepharoplasty Insurance Coverage
In some cases, health insurance companies will provide coverage for a blepharoplasty if the upper eyelid skin is so redundant that it obstructs your peripheral vision
It does require a thorough examination by a surgical specialist and objective documentation that lifting the eyelid skin will correct the visual field loss to a significant degree. Standardized photographs of your eyes are also usually necessary for review
Insurance will occasionally cover upper eyelid surgery.
Upper eyelid surgery is occasionally covered by insurance but it is getting harder and harder to get those cases approved. A visual field study that shows some impairment is usually required.
Blepharoplasty is covered if you meet criteria, depending on insurance company
Visually obstructive eyelid problems are absolutely included in most insurance companies’ benefits. An ophthalmology or oculoplastic surgeon has equipment in the office to measure the amount of visual obstruction from the eyelid problem. Based on the patient’s complaint, the visual field loss from the eyelids, and the photographic documentation, these upper eyelid procedures are frequently approved by Medicare and private insurance companies
If you are trying to have your eyelids “done” for looks, then it is a cosmetic procedure and not covered.
Can upper blepharoplasty be covered by insurance?
Upper eyelid surgery can sometimes be covered by insurance if vision is being impaired by the hooding over the eye. A exam of the vision is needed to determine if there is any impairment or not.
I would start with this exam to determine if you might be covered for the procedure or not.

Blepharoplasty Will Insurance Cover
Insurance applies only if it is medically necessary
There is no insurance coverage for Blepharoplasty surgery unless it affects the field of vision; even then it may not be covered. If not, it is considered cosmetic and elective surgery.
Cosmetic Blepharoplasty is not covered
If your upper eyelids cover your visual fields in a demonstrable way then insurance should cover it. However, you will need to go to an ophthalmologist to have visual field testing and these test do not lie
Lower eyelids may sag and cause eyelid dryness and this may be covered, but once again you will need to see a second opinion or jump through hoops in order to get this covered as well
Insurance Companies Will Cover Blepharoplasty Or Ptosis Repair
Insurance paying for upper eyelid surgery
There are three criteria that medicare has established and all three need to be documented before your insurance company considers covering the cost of upper eyelid surgery.
- Documentation of superior visual field loss: This test is performed with each eyelid taped up to prove improvements in the superior visual field after surgery
- Documentation of ptosis (eyelid droop) OR dermatochlasia by your surgeon
- Frontal and side view photographs documenting the presence of ptosis or dermatochlasia. Now remember each insurance company is different and may have their own rules for qualifications
Insurance coverage for Blepharoplasty
Insurance coverage generally does not pay for cosmetic procedures. They will, however, contemplate paying for reconstructive or functional surgery. That having been said, each company determines the parameters by which they establish medically necessary blepharoplasty using reconstructive and functional criteria
These are not consistent among insurance companies and no standard have been established. Generally, the indications for medically necessary blepharoplasty include blepharoptosis, blepharochalasis, or dermatochalasis. Other conditions include congenital (from birth), traumatic (from injury), or oncologic (from cancer) indications
One of the most common conditions involves excess upper eyelid skin,which hangs down and obstructs vision.
This is documented using the visual field testing referred to in the other physicians responses. Another condition called blepharoptosis is easily confused with above but is due to the upper eyelid (not the skin) covering the pupil
People confuse this with a tired or droopy eye look. It is usually associated with muscle problems that require repair. This can be documented with a photograph. Blepharoptosis can be present at birth or develop over time and effect one eye or both
Injuries to the eye may result in scars or abnormal conditions that require repair. Removal of skin cancers can also precipitate the need for reconstructive procedures.
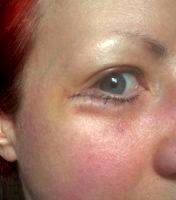
Medical Insurance Companies Rarely Pay For Cosmetic Blepharoplasty
Do You Qualify For Eyelid Surgery?
It is hard to answer that question without an examination. Some policies specifically exclude upper eyelid blepharoplasty and others have higher deductibles. United Health Care is not known to be one of the more generous insurance companies when it comes to this type of surgery.
Probably best to weigh the options and remember that at least some of this will be out of pocket. Having performed several thousand upper eyelid surgery procedures for functional and aesthetic reasons, very few “functional” surgery patients aren’t concerned about the aesthetic outcome of this surgery.
Upper lid surgery with insurance
This is not a great picture since it is not from the front although it looks like you may have enough dermatochalasis and possible ptosis to qualify for insurance coverage. You should see an oculoplastic surgeon who can evaluate your eyelids and determine what surgery you would need.
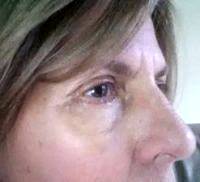
Medicare Or Your Private Health Insurance Likely Will Cover A Major Portion Of The Cost Of A Functional Blepharoplasty
A visual field test is then performed to see if there is a restriction in the vision due to the low lids. The visual field is then sent with photos to your insurance company if they give prior approval for surgeries.
Sometimes they will approve only part of what you may want and or need. you would then have to pay for the part that they consider cosmetic
You will need to see an opthalmologist to have a field of vision performed to see whether you vision to the side is compromised by the “hooding” effect of the upper eyelid skin (and ptotic eyebrows).
If that test is positive, then I would submit it to your insurance carrier to see whether they would approve the procedure and how much ($) they would cover. Make sure you have their response in writing.
More than likely, the insurance (if at all) will cover only the eyelid surgery and not the elevation of the brows (which will also improve the hooding effect).
Insurance Coverage for Upper Eyelid Surgery?
The short answer to your question is that it is possible that your insurance plan may cover your surgery in some cases. Commercial insurance plans do vary greatly in terms of their coverage for these procedures, even within the same company such as United Healthcare.
Many plans will closely follow the Medicare criteria for coverage, but this is not a certainty either, and there are wide geographic variations in these Medicare criteria depending on which Medicare carrier is in charge in your part of the country.

Most Insurance Companies Have Specific Guidelines Regarding Criteria For Covering Blepharoplasty
Additionally, we are seeing a larger number of commercial plans who now have “upper eyelid surgery” listed as a specific exclusion in the policy, in which case, there is absolutely no circumstance where the surgery would be covered by these plans.
Nowadays, this has made things even more confusing for doctors and patients alike, and it creates a very difficult situation for both parties even if an insurance company decides to “pre-authorize” a surgery without giving a firm “guarantee of payment.
“My advice would be for you to see a qualified Oculoplastic Surgeon in your area who is well-versed in the local Medicare requirements for insurance coverage, as these typically serve as a general guide for the requirements of commercial plans.
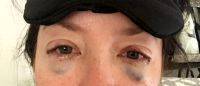
DOES INSURANCE COVER BLEPHAROPLASTY OR OTHER EYELID SURGERY
A part of your evaluation will include documentation of some specific history points, careful measurements of your eyelids, external photos, and visual field testing in some form. After this evaluation, you may be given a better idea of whether you would even be a candidate for insurance coverage for your surgery, but please remember that this is still not a guarantee that your insurance plan will pay for the surgery appropriately at the end of the day.
Insurance and eyelids
With each passing year insurance companies seem to become more restrictive in their criteria for coverage of surgical procedures that they may deem elective, but many carriers still define criteria by which upper eyelid surgery is covered.
They make the distinction between cosmetic procedures and functional procedures, and the burden is on the patient to prove that there are functional consequences to their droopy lids, namely restricted peripheral vision. Most providers require a set of photographs demonstrating descent of the lid skin past the lid margin, as well as visual field tests.
These tests, usually performed by an ophthalmologist, define how much of the world a patient sees when looking forward. The test can then be repeated with the lids taped, simulating surgery, and estimating the amount of improvement that can be anticipated.
Different providers and different policies have different thresholds for coverage.
Is upper eyelid drooping covered by insurance?
The answer is maybe. It is getting more and more difficult to get insurance companies to cover upper eyelid droopiness. The medical term for the procedure is upper eyelid blepharoplasty. The droopiness has to be so bad that it interferes with your vision.
Insurance companies often want you to go to an ophthalmologist to get what’s called visual field testing. If this testing shows that you have peripheral field vision loss and the eye doctor feels that it is due to your excess upper eyelid skin, your insurance company may consider it.
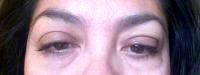
Most Insurance Companies Base Their Criteria Off Medicare Guidelines
It is best to have a conversation with your insurance company to see exactly what they require and then get it pre-approved. Good luck, it is very difficult to get them to give you the OK. (Franklin D. Richards, MD, Bethesda Plastic Surgeon)
Insurance might pay for upper eyelid surgery in exceptional cases.
Most insurance companies do not cover upper eyelid surgery. If the insurance company does they generally require that there be a visual field disturbance. Your plastic surgeon can sort this out for you. (Vincent N. Zubowicz, MD, Atlanta Plastic Surgeon)
Eyelid surgery and insurance
In some cases your insurance company will cover upper eyelid surgery. All insurance companies are different and require different criteria to cover the costs of surgery. I recommend you have a consultation with a board certified plastic surgeon to evaluate your eyelids. (Ross Stutman, MD, Scottsdale Plastic Surgeon)
